For many people living with arthritis and persistent musculoskeletal conditions, pain can be hard to describe with words alone. Some days it is intense; other days it moves, changes, or feels entirely different. It can be confronting, confusing, and at times unpredictable. No two people experience pain in the same way, it feels different to everyone.
Traditionally, pain was understood as a direct signal of tissue damage – something is “wrong,” and the body alerts us. 
However, advances in pain science have reshaped this understanding. We now know that pain is not simply a measure of injury, but a complex, dynamic experience influenced by the brain, nervous system, and a range of physical, psychological, and social factors.
Pain is Real, but not always about damage
Modern pain science shows that pain is produced by the brain as a protective response. This means:
- Pain does not always equal harm
- The intensity of pain does not always reflect the severity of tissue damage
- Pain can persist even after tissues have healed
In conditions like osteoarthritis, imaging findings (such as “bone-on-bone”) often don’t match a person’s pain levels. Some people with significant joint changes report little pain, while others with minimal changes experience severe symptoms.
This highlights a key message: pain is real, but it is not always a reliable indicator of structural damage, therefore should not discourage you from exploring different pain management strategies.
Understanding the Nervous System
Persistent pain is often linked to changes in how the nervous system processes signals, sometimes referred to as sensitization.
Over time, the nervous system can become more protective, meaning:
- Pain signals are amplified
- The threshold for triggering pain is lowered
- Even safe movements may feel painful
This is not “in your head” it is a biological response involving the brain and spinal cord.
The Role of the Brain in Pain
The brain continuously evaluates threats based on:
- Past experiences
- Beliefs and expectations
- Stress levels
- Sleep quality
- Emotional wellbeing
If the brain perceives a higher level of threat, it can increase pain output, even in the absence of new injury. This is why factors like poor sleep, stress, or fear of movement can worsen pain. The nervous system is constantly tracking these and when these stressors are not resolved, it accumulates and over time the baseline changes. Eventually, there will be a threshold where the nervous system cannot absorb any more stress, which is when more symptoms begin to surface.
What This Means for Pain Relief
The good news is that the human body is incredibly adaptable. Understanding pain science opens the door to more effective, evidence-based strategies for relief. Rather than focusing solely on the joint or area of pain, this is why a whole-person approach is more powerful than we think.
1. Movement is Medicine
Gentle, regular movement helps:
- Calm the nervous system
- Improve joint function
- Build confidence and reduce fear of movement
When we are stressed, the body activates its fight-or-flight response, increasing muscle tension as a protective mechanism. In short bursts, this is helpful but when stress becomes chronic, muscles can remain in a persistently tightened state.
This ongoing tension can:
- Increase pain and stiffness
- Reduce blood flow to muscles
- Contribute to fatigue and discomfort
- Heighten sensitivity in the nervous system
Activities like walking, strength training, or Pilates can be highly effective when tailored to the individual.
2. Education Reduces Pain
Research shows that understanding how pain works can:
- Reduce fear and catastrophising
- Improve coping strategies
- Lead to better outcomes
Pain education, often referred to as pain neuroscience education, helps people reconceptualise pain as a protective response from the nervous system, rather than a direct sign of damage. This shift in understanding can have powerful effects on both the brain and body. This is why pain education is now considered a core component of treatment for chronic musculoskeletal conditions, including osteoarthritis.
It is often delivered alongside:
- Exercise and movement therapy
- Psychological strategies (such as cognitive behavioural approaches)
- Lifestyle support (sleep, stress, and overall health)
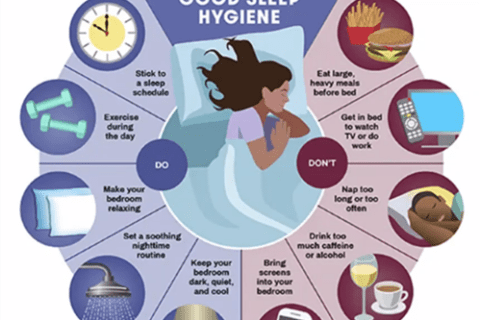
3. Sleep and Stress Matter
Poor sleep and chronic stress can increase pain sensitivity. When sleep is poor or stress is high:
- The nervous system becomes more sensitised
- Pain signals are amplified
- Recovery and tissue repair are reduced
- Mood and coping capacity decline
This can easily create a cycle where pain disrupts sleep, and poor sleep further worsens pain. Supporting:
- Good sleep habits
- Stress management techniques (e.g. mindfulness, relaxation)
can have a measurable impact on pain levels by helping shift the nervous system toward a more restorative, calm state.
4. Pacing and Consistency
Balancing activity and rest known as pacing helps prevent flare-ups and supports long-term progress. Consistency is more important than intensity.
A New Way Forward
Pain science shifts the conversation from “What is damaged?” to “What is driving the pain experience?”
This approach empowers people to move away from fear and toward active self-management building confidence, resilience, and long-term relief.
If you’re living with ongoing pain, understanding how pain works is one of the most powerful tools you can have. With the right support and strategies, it is possible to reduce pain and improve quality of life.